Abstract
Background: Chronic pain conditions and mental disorders have high prevalence rates in military populations. However, few investigations have examined the comorbidity between chronic pain conditions and specific mental disorders among Canadian active military personnel.
Methods: We conducted a secondary analysis of data from the 2013 Canadian Forces Mental Health Survey (CFMHS) concerning the population of regular members. Diagnostic interviews assessed the presence of mental disorders, and participants self-reported chronic pain conditions (i.e., arthritis, back problems, musculoskeletal conditions, migraines) and indicators of pain severity. We used multiple logistic regressions to assess associations between chronic pain conditions and mental disorders. We used cross-tabulations to assess the prevalence of pain severity indicators in comorbid relationships compared with the chronic pain condition alone. We used moderation analyses to examine the interactions between pain condition by pain severity, and pain condition by activity limitation, respectively, on mental disorders.
Results: The CFMHS included data from 6696 regular members and had a response rate of 79.8%. About one-quarter (n = 1761) of military personnel reported having chronic pain. In the fully adjusted model, all assessed pain conditions were significantly associated with posttraumatic stress disorder (PTSD) (odds ratio [OR] range 1.86–2.55), and several pain conditions were associated with major depressive episode, generalized anxiety disorder and panic disorder. Back problems were significantly associated with all mental disorders apart from alcohol use disorders (OR range 1.40–2.17). Cross-tabulations showed higher prevalence estimates of endorsement for pain severity indicators among pain conditions and comorbid mental disorders, compared with pain conditions alone. Formal moderation analyses showed a significant relationship between migraine and activity limitation on PTSD.
Interpretation: Chronic pain conditions are prevalent and co-occur with mental disorders among Canadian regular force members. Greater understanding of these chronic pain conditions and mental disorders and their impact on people’s abilities to adapt to both military and civilian life is needed.
Chronic pain, physical conditions and mental disorders are prevalent among military personnel. Chronic pain estimates in former members of the Canadian Armed Forces (CAF) are estimated to be about 41%.1 Although some research has shown higher chronic pain estimates in the Canadian veteran population compared with the general population,2 other studies have shown comparable prevalence estimates among the two populations.3 In addition, there are no recent estimates of the prevalence of chronic pain in the serving CAF.
Canadian regular force veterans have higher rates of conditions characterized by pain, including arthritis, back pain and bowel disorders compared with the general population.4 High estimates of mental health conditions are also seen. In 2002, the Canadian Community Health Survey Canadian Forces Supplement (CCHS-CF) showed significantly higher past-year prevalence rates of depression and panic disorder among regular members of the CAF compared with the rates seen in the general population.5 High prevalence rates in the CAF are corroborated by more recent research, with the prevalence of general anxiety disorder being twice as high as that of the general population in 2008.4
Interest in the relationship between mental disorders and pain conditions is growing. General population–based studies have found strong relations between chronic physical pain conditions and depression,6–10 anxiety disorders11–13 and posttraumatic stress disorder (PTSD)14–16 among other mental disorders.17 Comorbid physical and mental conditions are associated with greater disability and activity limitation compared with a single condition alone,18–20 which suggests that the presence of physical pain may moderate these associations. Further, research has shown a significant association between chronic pain and certain mental disorders.20 However, a limitation of these studies is the lack of research looking at specific mental disorders; research examining comorbid relationships has primarily examined summary disorder categories. Lack of research examining chronic pain severity as a potential mechanism or differentiating factor for these comorbid relations is an additional limitation. Assessing pain severity would provide a better understanding of the role mental disorders have on the prevalence of pain severity and activity limitations among people with pain conditions. There are even greater gaps within the military context regarding comorbidity research. Research involving the military population has primarily focused on PTSD and its relationship with physical conditions.14,15,21 Furthermore, there is limited research within the Canadian military context regarding these comorbidities, particularly among active duty personnel. Here, we address many of these limitations by investigating the relations between specific mental disorders, chronic pain severity and pain conditions in a contemporary sample population of active military personnel in Canada.
Our objectives were to estimate the prevalence of chronic pain and physical conditions characterized by pain among Canadian military personnel, examine the association between pain conditions and mental disorders and assess severity indicators of chronic pain between comorbid pain conditions and mental disorders.
Methods
Data source and study population
We conducted a secondary analysis of data drawn from the cross-sectional 2013 Canadian Forces Mental Health Survey (CFMHS) conducted by Statistics Canada. The CFMHS sample population was a nationally representative sample of regular force members and a nonrepresentative sample of reserve force members.22 For this reason, we included only regular force members in our study. Statistics Canada stratified the sample by deployment status and rank to ensure representativeness of the regular force members.22
Interviewers surveyed respondents face-to-face using a computer-assisted interviewing technique. Survey questions were based partly on the World Mental Health Survey, the Canadian Community Health Survey (CCHS; cycle 5.2) and other special surveys.22 Qualitative testing of the questionnaire was conducted in 2011 to evaluate respondents’ understanding of the survey and assess their willingness and ability to provide information.22 Statistics Canada used a complex sampling design to ensure representativeness. Consent was given by respondents before the start of the survey. Data were collected between Apr. 15 and Aug. 31, 2013.22
Primary variables
Mental disorders
The World Health Organization version of the Composite International Diagnostic Interview (WHO-CIDI)23 based on Diagnostic and Statistical Manual of Mental Disorders-IV (DSM-IV)24 and the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10) criteria assessed past-year mental disorders. Codes for major depressive episode (MDE), GAD, panic disorder, PTSD and alcohol use disorder (AUD) were included in the analysis.23 Research has shown concordance between the WHO-CIDI and Structured Clinical Interviews for DSM-IV (SCID).25
Pain conditions
Physical conditions in this study included those that were frequently characterized by pain, were expected to last or had already lasted at least 6 months and were based on self-report of having been diagnosed by a health professional. Pain conditions included arthritis; back problems excluding fibromyalgia and arthritis; other musculoskeletal problems and fibromyalgia; and migraine headaches. An “any pain condition” variable was computed for any respondents who reported 1 or more pain conditions. Physical conditions such as asthma and diabetes — included within the CFMHS — were not included within this study because they are not primarily characterized by pain, and because they have low prevalence rates within this young adult population. Gastrointestinal diseases were not assessed in the CFMHS.
Chronic pain characteristics
Among all respondents, the presence of chronic pain was assessed using the question “Are you usually free of pain or discomfort,” with self-reported “no” answers suggesting chronic pain. Pain was further characterized by severity and the number of activities prevented. Pain severity was assessed by a description of the usual intensity of their pain or discomfort: “mild,” “moderate” or “severe.” The respondent was able to select from 4 options (none, a few, some, most) to describe the number of activities prevented owing to pain or discomfort. This style of question regarding activity limitation has been used in several iterations of the CCHS and has been used to assess the prevalence of chronic pain within the general population.3 We created the following categorizations based on prevalent responses and sensitivity analyses: “no pain and mild pain” or “moderate and severe pain” for pain severity, and “no pain, none or a few” activities prevented or “some to most” activities prevented.
Sociodemographic and military variables
Sociodemographic variables included age (assessed continuously), sex, marital status (married or common-law; separated, divorced or widowed; single, never married), education level (high school or less; some postsecondary; trade, college, or university certificate or diploma; university degree), household income (≤ $29 999; $30 000–$49 999; $50 000–$79 999; ≥ $80 000) and ethnicity (white, other). Military-related variables include rank (junior noncommissioned member, senior noncommissioned member, officer) and CAF element (army, navy, air force). Marital status and income were categorized in accordance with other literature that has used the CFMHS;26 education level, ethnicity and military rank were derived variables created by Statistics Canada.
Analytical strategy
We used cross-tabulations to derive frequencies for the presence of chronic pain among each physical condition and the presence of individual mental disorders (i.e., major depressive episode, generalized anxiety disorder, panic disorder, PTSD, AUD) among each pain condition. We used bivariate (model 1) and multiple logistic regression models to assess the relation between pain conditions (independent variable) and each mental disorder (dependent variable). We adjusted multivariable models for sociodemographic factors (age, sex, marital status, education level, income, ethnicity, rank, CAF element) (model 2), and for sociodemographic factors and mental disorders (excluding the disorder of interest) (model 3).
To examine the effect of pain severity in comorbid relations, we used cross-tabulations to examine the proportion of respondents who reported severe versus mild pain severity and activity limitation, with and without the mental disorder of interest, for each pain condition. This was done only among the pain conditions that were significantly associated with mental disorders in the fully adjusted logistic regression model. We then conducted a moderation analysis by entering the main effects and interaction terms into the same model to test the significance of the relations between pain condition by pain severity and pain condition by activity limitation with each mental disorder. To ensure representativeness of the CAF regular force, we weighted analyses using final probability weights derived from Statistics Canada and adjusted for nonresponse and the exclusion of out-of-scope units.27 We applied bootstrapping for variance estimation to account for the complex survey design using 500 replicate weights supplied by Statistics Canada. We conducted all analyses in STATA software.28
Ethics approval
Ethical approval to conduct the survey was obtained through the relevant bodies within Statistics Canada.27
Results
Sample description
The CFMHS included data from 6696 regular members of the CAF, and had a response rate of 79.8%.25 Table 1 includes a description of the sample. The mean age of included respondents was 35 years, and most respondents were male (86.1%, n = 5773). The army was the most prevalent CAF element in the sample (53.1%, n = 3459), and junior noncommissioned member was the most prevalent rank (55.0%, n = 2816). About one-quarter of the respondents indicated chronic pain or discomfort (25.5%, n = 1761); of these respondents, more than 60% (n = 1102) deemed their pain to be moderate to severe. “Other musculoskeletal problems and fibromyalgia” was the most prevalent pain condition (30.5%, n = 2130), and 46.7% (n = 3243) of respondents had any pain condition.
Characteristics of included respondents
Cross-tabulations to examine the presence of chronic pain among each condition showed that, of respondents with arthritis, 70.1% (weighted n = 5380 out of 7680 with arthritis) reported chronic pain, followed by back problems (57.8%, weighted n = 8660 out of 14980), other musculoskeletal problems and fibromyalgia (51.5%, weighted n = 10 100 out of 19 600) and migraine (47.3%, weighted n = 2780 out of 5880) (data not shown).
Comorbidities
Table 2 shows the prevalence of mental disorders among each pain condition. All pain conditions were significantly associated with major depressive episode, generalized anxiety disorder and panic disorder in both model 1 and model 2. Once adjusted for other mental disorders, only PTSD remained significantly associated with all pain conditions (model 3 odds ratio [OR] range 1.86–2.55); however, major depressive episode, generalized anxiety disorder and panic disorder remained significantly associated with some pain conditions. No significant relations were seen between alcohol use disorder and pain conditions in the fully adjusted model.
Logistic regressions analyzing the relations between pain conditions and past-year mental disorders among Canadian Armed Forces personnel
Pain severity analyses
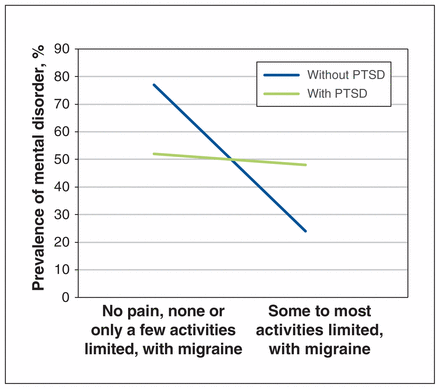
Cross-tabulations calculated on the significant regression results of the fully adjusted model showed that, among the pain conditions, a larger proportion of respondents endorsed severe pain when the mental disorder of interest was present, compared with when it was not (Table 3). Similar results were seen with regard to activity limitation, with the presence of a mental disorder yielding higher proportions of greater activity limitations compared with those with the pain condition alone. When conducting formal interaction analyses, a significant relation was seen only between migraine and activity limitation on PTSD (p < 0.05) (Figure 1). No other interaction analyses between physical conditions, mental disorders and activity limitation reached significance.
Proportions of endorsed chronic pain severity indicators among those with a pain condition with and without the mental disorder of interest
Formal interaction analysis between migraine and activity limitation in posttraumatic stress disorder (PTSD).
Interpretation
In our investigation that examined mental and physical health comorbidities and the effect of chronic pain among the active regular force members of the CAF, 25% of the included respondents reported regular chronic pain. The strength of the association between pain conditions and mental disorders varied depending on the disorder, with robust findings for PTSD. Among respondents with a pain condition, trends emerged that suggest higher estimates of more severe pain indicators — in terms of both pain severity and activity limitation — in respondents with a comorbid mental disorder compared with those without.
As seen among members released from the CAF,29 chronic pain is common among active members of the CAF (25.5%), with most respondents reporting their pain as moderate to severe. Indeed, 75% of members with chronic pain reported some impact on functioning. High rates of pain conditions were also found and may be explained by the physically intensive work demands of the participants. Military work is often unpredictable and demanding,30 and deployed soldiers endure high rates of non-battle injury31 and poly-traumatic injuries.32 Pain conditions could be sequelae of past injuries, considering that injury-induced arthritis33 and injury-related disc degeneration34 do occur. Migraines and other back problems could also be related to injury.35,36
We identified 2 unique comorbidity trends: nonsignificant relations between physical conditions and alcohol use disorder and robust findings related to PTSD. Alcohol use is associated with chronic physiologic disease;37 however, the nature of the study population could explain our nonsignificant findings. Alcohol use disorder — a functionally impairing disorder — may not manifest in a population who are capable of working as active militants, suggesting lower drinking impairment. This explanation is likely, given the prevalence of alcohol use disorder is lower in the regular force population compared with the general population.38 This may be particularly true for personnel with pain conditions, where the combination may result in an inability to work.
Unlike alcohol use disorder, PTSD had strong associations with all assessed pain conditions, paralleling trends seen in the general population.39 PTSD may be associated with a pain condition through its symptom profile or through a secondary mechanism such as maladaptive behaviour. For example, sleep disturbance is commonly seen in PTSD,40 is associated with physical illness41–45 and is often seen in veterans,46 making poor sleep a possible propagating factor. Escape-avoidance behaviours (drinking, smoking, etc.) are used to cope after trauma,47,48 and are associated with several health conditions. 49–53 Deployment may prompt these behaviours,54 corroborated by increased smoking incidences in deployed compared with nondeployed personnel.55 Additional possible mechanisms may include physiologic indicators (e.g., increases in proinflammatory cytokines after exposure to stress) or genetic factors.56 Back problems remained significant with most mental disorders in the fully adjusted model, possibly owing to the heterogeneity of the group or the psychosomatic features indicated in back pain.57
Among significantly related mental and physical health conditions, cross-tabulations showed increased pain severity indicators among respondents with comorbid physical and mental health conditions compared with those with a physical condition alone. This trend was again particularly robust for PTSD. Although PTSD emerged as a robust indicator, the importance of investigating individual mental disorders among this population is supported; significant associations between physical conditions and several mental disorders remained present in the fully adjusted model, which accounted for sociodemographic factors and mental disorders (excluding the disorder of interest). Moreover, non-PTSD psychiatric disorders have been shown to be similarly disabling compared with PTSD in military populations.58,59
Limitations
A cross-sectional survey design was used, therefore causal inferences cannot be made. In addition, reliance on self-reported pain conditions may result in biased estimates, particularly for physical conditions that are inadequately defined (e.g., back problems, musculoskeletal problems), thereby possibly inflating estimates of these pain conditions. However, some research has shown a high concordance between self-reported physical conditions and physician-diagnosed conditions.60
Missing data could result in response bias, which should be considered when interpreting our results. Finally, focusing on the the survey sample narrows generalizability of our findings to all regular force members of the CAF. Furthermore, with most of the participants in our sample being male, our findings may be less generalizable to female military personnel.
Conclusion
A substantial number of regular force personnel have chronic physical health conditions often associated with chronic pain. Furthermore, there is high comorbidity between pain conditions and mental disorders, particularly PTSD. An emphasis on screening for mental disorders (particularly in the context of pain conditions) and prompt management of pain conditions in the primary care setting in the CAF is implied. Longitudinal research examining the development of comorbid mental and pain conditions within this population should be a priority. Moreover, these health conditions continue to persist after members are released from service.18 Thus, greater understanding of these comorbidities and their impact on people’s abilities to adapt to military and civilian life is needed.
Acknowledgements
The authors thank Jordana Sommer and Kayla Kilborn for their contributions.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Everett Vun contributed to the conception, design, acquisition of data, analysis, drafting and revising the article; Sarah Turner contributed to the acquisition of data, analysis, interpretation, drafting and revision of the article; Jitender Sareen contributed to the conception, design, acquisition of data, interpretation of data and revision of the article; Natalie Mota contributed to the design, interpretation and revision of the article; Tracie Afifi contributed to the design, interpretation and revision of the article; Renée El-Gabalawy contributed to the conception, design, acquisition of data, analysis, interpretation of data, revisions of the article and gave final approval for the version to be submitted. All of the authors approved the final version of the article and agreed to act as guarantors of the results.
Funding: This study was supported by the Mary E. Hedley Bequest, a research contract from the Government of Canada (Sareen), University of Manitoba Start-Up funds and internal funds from the Department of Anesthesiology, Perioperative and Pain Medicine, and the Canadian Institutes of Health Research Chronic Pain Network (El-Gabalawy).
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/6/4/E528/suppl/DC1.
References
- Copyright 2018, Joule Inc. or its licensors