Abstract
Background
This study was conducted to investigate whether annual surgical unit caseload affects extent of breast cancer surgery, breast cancer recurrence or breast cancer-specific survival.
Methods
In a population-based cohort study, 12,604 women diagnosed with breast cancer in Finland during the years 1998–2001 were followed up until the end of year 2008. Surgical units were divided into subgroups: >200, 100–200, 50–99 or <50 breast cancer operations per year. Information on patients, treatment, and follow-up was obtained from two national registries. The analyses were adjusted for age and disease stage. The reliability of the registry information was validated by comparison with information from one hospital area. Cox proportional hazard and logistic regression models were employed in the analyses.
Results
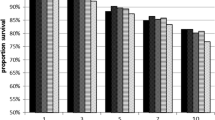
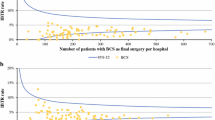
Validation of the registry data showed that date of diagnosis, age, stage, extent of surgery, and date and cause of death were reliably recorded in the registers. Information on radiotherapy was obtained by combining different registry data. Data on local and distant recurrences were not reliable enough to allow analyses. Patients in hospitals with smaller caseloads underwent mastectomy more often than those operated in hospitals with higher caseloads (P < 0.001). Higher caseloads were also related to improved survival (P = 0.031).
Conclusions
National registries should include information on both local and distant recurrences in order to provide reliable population-based data for evaluation of treatment results. Centralization of surgery to high-volume centers is supported by a higher incidence of conservative surgery and better survival.


Similar content being viewed by others
References
Fisher B, Anderson S, Bryant J, et al. Twenty-year follow up of a randomized trial comparing mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med. 2002;347:1233–41.
Veronesi U, Cascinelli N, Mariani L, et al. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med. 2002;347:1227–32.
Veronesi U, Paganelli G, Viale G et al. A randomized comparison of sentinel node biopsy with routine axillary dissection in breast cancer. N Engl J Med. 2003;349:546–53.
Nattinger A, Laud P, Sparapani R, Zhang X, Neuner J, Gilligan M. Exploring the surgeon volume-outcome relationship among women with breast cancer. Arch Intern Med. 2007;18:1958–63.
Harcourt KF, Hicks KL. Is there a relationship between case volume and survival in breast cancer? Am J Surg. 2003;185:407–10.
Stefoski M, Haward RA, Johnston C, Sainsbury R, Forman D. Surgeon workload and survival from breast cancer. Br J Cancer. 2003;89:487–91.
Kingsmore D, Hole D, Gillis C. Why does specialist treatment of breast cancer improve survival? The role of surgical management. Br J Cancer. 2004;90:1920–5.
Hebert-Croteau N, Brisson J, Lemaire J, Latreille J, Pineault R. Investigating the correlation between hospital of primary treatment and the survival of women with breast cancer. Cancer. 2005;104:1343–8.
Richards M, Sainsbury R, Kerr D. Inequalities in breast cancer care and outcome. Br J Cancer. 1997;76:634–8.
Sainsbury R, Haward B. Influence of clinician workload and patterns of treatment on survival from breast cancer. Lancet. 1995;345:1265–70.
Finnish Cancer Registry. Cancer in Finland 2006 and 2007. Cancer Society of Finland Publ No 76. Helsinki; 2009.
Lee-Feldstein A, Anton-Culver H, Feldstein PJ. Treatment differences and other prognostic factors related to breast cancer survival. Delivery systems and medical outcomes. JAMA. 1994;271:1163–8.
Allgood PC, Bachmann MO. Effects of specialization on treatment and outcomes in screen-detected breast cancers in Wales: cohort study. Br J Cancer. 2006;94:36–42.
Houssami N, Sainsbury R. Breast cancer: multidisciplinary care and clinical outcomes. Eur J Cancer. 2006;42:2480–91.
Skinner KA, Helsper JT, Deapen D, Ye W, Sposto R. Breast cancer: do specialists make a difference? Ann Surg Oncol. 2003;10:606–15.
Roohan PJ, Bickell NA, Baptiste MS, Therriault GD, Ferrara EP, Siu AL. Hospital volume differences and five-year survival from breast cancer. Am J Public Health. 1998;88:454–7.
Golledge J, Wiggins JE, Callam MJ. Effect of surgical subspecialization on breast cancer outcome. Br J Surg. 2000;87:1420–5.
Gillis CR, Hole DJ. Survival outcome of care by specialist surgeons in breast cancer: a study of 3786 patients in the west of Scotland. BMJ. 1996;312:145–8.
Guller U, Safford S, Pietrobon R, Heberer M, Oertli D, Jain NB. High hospital volume is associated with better outcomes for breast cancer surgery. Analysis of 233,247 patients. World J Surg. 2005;29:994–9.
Neuner JM, Gilligan MA, Sparapani R, Laud PW, Haggstrom D, Nattinger AB. Decentralization of breast cancer surgery in the United States. Cancer. 2004;101:1323–9.
Montazeri A. Health-related quality of life in breast cancer patients: a bibiliographic review of the literature from 1974 to 2007. J Exp Clin Cancer Res. 2008;27:32.
Acknowledgment
We want to thank the Medical Research Fund of Tampere University Hospital (9J018, 9K028, 9L079), the Academy of Finland, and Elna Kaarina Savolainen’s legacy funds for development of cancer patient care for their financial support. We owe our sincere thanks to the Finnish Cancer Registry for their cooperation, to Mrs. Heini Huhtala, MSc, for valuable statistical assistance and to Mrs. Kirsi Rouhento for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Peltoniemi, P., Peltola, M., Hakulinen, T. et al. The Effect of Hospital Volume on the Outcome of Breast Cancer Surgery. Ann Surg Oncol 18, 1684–1690 (2011). https://doi.org/10.1245/s10434-010-1514-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1514-1