Abstract
BACKGROUND: Bedside rationing by physicians is controversial. The debate, however, is clouded by lack of information regarding the extent and character of bedside rationing.
DESIGN, SETTING, AND PARTICIPANTS: We developed a survey instrument to examine the frequency, criteria, and strategies used for bedside rationing. Content validity was assessed through expert assessment and scales were tested for internal consistency. The questionnaire was translated and administered to General Internists in Norway, Switzerland, Italy, and the United Kingdom. Logistic regression was used to identify the variables associated with reported rationing.
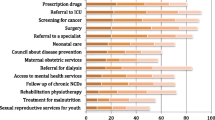
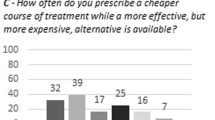
RESULTS: Survey respondents (N=656, response rate 43%) ranged in age from 28 to 82, and averaged 25 years in practice. Most respondents (82.3%) showed some degree of agreement with rationing, and 56.3% reported that they did ration interventions. The most frequently mentioned criteria for rationing were a small expected benefit (82.3%), low chances of success (79.8%), an intervention intended to prolong life when quality of life is low (70.6%), and a patient over 85 years of age (70%). The frequency of rationing by clinicians was positively correlated with perceived scarcity of resources (odds ratio [OR]=1.11, 95% confidence interval [CI] 1.06 to 1.16), perceived pressure to ration (OR=2.14, 95% CI 1.52 to 3.01), and agreement with rationing (OR=1.13, 95% CI 1.05 to 1.23).
CONCLUSION: Bedside rationing is prevalent in all surveyed European countries and varies with physician attitudes and resource availability. The prevalence of physician bedside rationing, which presents physicians with difficult moral dilemmas, highlights the importance of discussions regarding how to ration care in the most ethically justifiable manner.
Similar content being viewed by others
References
Asch DA, Ubel PA. Rationing by any other name. N Engl J Med. 1997;336:1668–71.
Relman A. Use of medical resources—overview. Prev Med. 1990;19:688–92.
Bloche MG, Jungman ER. The “R” word. J Contemp Health Law Policy. 2002;18:633–9.
Coulter A, Ham C. The Global Challenge of Health Care Rationing. Buckingham: Open University Press; 2000.
Sulmasy DP. Physicians, cost control, and ethics. Ann Intern Med. 1992;116:920–6.
Hiatt HH. Protecting the medical commons: who is responsible? N Engl J Med. 1975;293:235–41.
Loewy EH. Cost should not be a factor in medical care. N Engl J Med. 1980;302:697.
Levinski N. The doctor’s master. N Engl J Med. 1983;311:1573–5.
Pellgrino ED. Managed care at the bedside: how do we look in the moral mirror? Kennedy Inst Ethics J. 1997;7:321–30.
Askin WJ. Bedside rationing. CMAJ. 2002;166:711.
Weinstein MC. Should physicians be gatekeepers of medical resources? J Med Ethics. 2001;27:268–74.
Veatch RM. Who should manage care? The case for patients. Kennedy Inst Ethics J. 1997;7:391–401.
Morreim E. Balancing Act; The New Medical Ethics of Medicine’s New Economics. Dordrecht: Kluwer Academic Publishers; 1991.
Pearson SD. Caring and cost: the challenge for physician advocacy. Ann Intern Med. 2000;133:148–53.
Ubel P. Pricing Life: Why It’s Time for Health Care Rationing. Cambridge, MA: The MIT Press; 2001:(McGee G, Caplan A, eds. Basic Bioethics).
Daniels N. What is the obligation of the medical profession in the distribution of health care? Soc Sci Med [F]. 1981;15F:129–33.
Baines DL, Tolley KH, Whynes DK. The ethics of resource allocation: the views of general practitioners in Lincolnshire, U.K. Soc Sci Med. 1998;47:1555–64.
Cooke L, Hutchinson M. Doctors’ professional values: results from a cohort study of United Kingdom medical graduates. Med Educ. 2001;35:735–42.
Rosen P, Karlberg I. Opinions of Swedish citizens, health-care politicians, administrators and doctors on rationing and health-care financing. Health Expect. 2002;5:148–55.
van Delden JJ, Vrakking AM, van der Heide A, van der Maas PJ. Medical decision making in scarcity situations. J Med Ethics. 2004;30:207–11.
Ubel PA, Baron J, Nash B, Asch DA. Are preferences for equity over efficiency in health care allocation “all or nothing”? Med Care. 2000;38:366–73.
Perneger TV, Martin DP, Bovier PA. Physicians’ attitudes toward health care rationing. Med Decis Making. 2002;22:65–70.
Ryynanen OP, Myllykangas M, Kinnunen J, Takala J. Doctors’ willingness to refer elderly patients for elective surgery. Fam Pract. 1997;14:216–9.
Escher M, Perneger TV, Chevrolet JC. National questionnaire survey on what influences doctors’ decisions about admission to intensive care. BMJ. 2004;329:425.
Mendelssohn DC, Kua BT, Singer PA. Referral for dialysis in Ontario. Arch Intern Med. 1995;155:2473–8.
Wilson R, Godwin M, Seguin R, et al. End-stage renal disease: factors affecting referral decisions by family physicians in Canada, the United States, and Britain. Am J Kidney Dis. 2001;38:42–8.
Arnesen T, Fredriksen S. Coping with obligations towards patients and society: an empirical study of attitudes and practice among Norwegian physicians. J Med Ethics. 1995;21:158–61.
WHO. Countries: selected indicators. Vol. 2005; 2003. Available at: http://www.who.int/countries/en/.
Ubel PA, Goold SD. ‘Rationing’ health care. Not all definitions are created equal. Arch Intern Med. 1998;158:209–14.
Sulmasy DP, Bloche MG, Mitchell JM, Hadley J. Physicians’ ethical beliefs about cost-control arrangements. Arch Intern Med. 2000;160:649–57.
Ryynanen OP, Myllykangas M, Kinnunen J, Takala J. Attitudes to health care prioritisation methods and criteria among nurses, doctors, politicians and the general public. Soc Sci Med. 1999;49:1529–39.
DuVal G, Clarridge B, Gensler G, Danis M. A national survey of U.S. internists’ experiences with ethical dilemmas and ethics consultation. J Gen Intern Med. 2004;19:251–8.
Hurst SA, Hull SC, DuVal G, Danis M. Physicians’ responses to resource constraints. Arch Intern Med. 2005;165:639–44.
Edwards P, Roberts I, Clarke M, et al. Increasing response rates to postal questionnaires: systematic review. BMJ. 2002;324:1183.
Asch DA, Jedrziewski MK, Christakis NA. Response rates to mail surveys published in medical journals. J Clin Epidemiol. 1997;50:1129–36.
Alexander GC, Werner RM, Ubel PA. The costs of denying scarcity. Arch Intern Med. 2004;164:593–6.
Wennberg JE, MacAndrew Cooper M. The Quality of Medical Care in the United States: a Report on the Medicare Program; the Dartmouth Atlas of Health Care 1999. Chicago, IL: AHA Press; 1999.
OECD. Health Data 2005. 2005.
Herzlinger RE, Parsa-Parsi R. Consumer-driven health care: lessons from Switzerland. JAMA. 2004;292:1213–20.
Committee on Consequences of Uninsurance. Insuring Health: Care Without Coverage: Too Little Too Late. Washington, DC: National Academy Press; 2002:(Institute of Medicine, ed).
Wynia MK, VanGeest JB, Cummins DS, Wilson IB. Do physicians not offer useful services because of coverage restrictions? Health Aff (Millwood). 2003;22:190–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
The views expressed here are the authors’ own and do not reflect the position of the National Institutes of Health, of the Public Health Service, or of the Department of Health and Human Services.
Conflict of interest statement for authors: none
This work was funded by the Department of Clinical Bioethics at the National Institutes of Health, and was conducted while S.A.H. was a fellow at this Department. S.A.H. was funded in part by the University Hospitals of Geneva, by the Oltramare Foundation, and by the Centre Lémanique d’Ethique. The views expressed here are the authors’ own, and not necessarily those of the University Hospitals of Geneva, the Oltramare Foundation, or the Centre Lémanique d’Ethique.
The funding sources were not involved in the study design, the collection, analysis, or interpretation of data, in the writing of the report, or in the decision to submit the paper for publication.
S.A.H. had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Rights and permissions
About this article
Cite this article
Hurst, S.A., Slowther, AM., Forde, R. et al. Prevalence and determinants of physician bedside rationing. J Gen Intern Med 21, 1138–1143 (2006). https://doi.org/10.1111/j.1525-1497.2006.00551.x
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2006.00551.x