Abstract
Background: British Columbia’s 8-1-1 telephone service connects callers with nurses for health care advice. As of Nov. 16, 2020, callers advised by a registered nurse to obtain in-person medical care can be subsequently referred to virtual physicians. We sought to determine health system use and outcomes of 8-1-1 callers urgently triaged by a nurse and subsequently assessed by a virtual physician.
Methods: We identified callers referred to a virtual physician between Nov. 16, 2020, and Apr. 30, 2021. After assessment, virtual physicians assigned callers to 1 of 5 triage dispositions (i.e., go to emergency department [ED] now, see primary care provider within 24 hours, schedule an appointment with a health care provider, try home treatment, other). We linked relevant administrative databases to ascertain subsequent health care use and outcomes.
Results: We identified 5937 encounters with virtual physicians involving 5886 8-1-1 callers. Virtual physicians advised 1546 callers (26.0%) to go to the ED immediately, of whom 971 (62.8%) had 1 or more ED visits within 24 hours. Virtual physicians advised 556 (9.4%) callers to seek primary care within 24 hours, of whom 132 (23.7%) had primary care billings within 24 hours. Virtual physicians advised 1773 (29.9%) callers to schedule an appointment with a health care provider, of whom 812 (45.8%) had primary care billings within 7 days. Virtual physicians advised 1834 (30.9%) callers to try a home treatment, of whom 892 (48.6%) had no health system encounters over the next 7 days. Eight (0.1%) callers died within 7 days of assessment with a virtual physician, 5 of whom were advised to go to the ED immediately. Fifty-four (2.9%) callers with a “try home treatment” disposition were admitted to hospital within 7 days of a virtual physician assessment, and no callers who were advised home treatment died.
Interpretation: This Canadian study evaluated health service use and outcomes arising from the addition of virtual physicians to a provincial health information telephone service. Our findings suggest that supplementation of this service with an assessment from a virtual physician safely reduces the overall proportion of callers advised to seek urgent in-person visits.
All Canadian provinces have nurse-managed, telephone services to support the public with health concerns (e.g., https://healthconnectontario.health.gov.on.ca/static/guest/home).1 These also exist in other jurisdictions, and provide guidance on management and the need for in-person care.2–5 In 2008, British Columbia established an 8-1-1 line, overseen by HealthLink BC, where nurses use standardized algorithms to provide advice ranging from home management to immediate emergency department (ED) attendance. Of the 948 793 BC callers to 8-1-1 in 2021, 328 537 were referred to a nurse and 91 662 of those (27.9%) were initially triaged to seek immediate care at an ED or physician office (Sandra Sundhu, HealthLink BC, Victoria: unpublished data, 2021). The COVID-19 pandemic greatly increased both the volume and complexity of calls to 8-1-1 in BC, with many callers seeking to avoid the perceived risk of in-person visits. This prompted HealthLink BC, in collaboration with the BC Emergency Medicine Network, to add a service for consultation with a virtual physician on Apr. 6, 2020, called HealthLink BC Emergency iDoctors in Assistance (HEiDi).6 Callers identified by an 8-1-1 nurse as having a concern of sufficient urgency to require medical attention within 24 hours can now be referred for optional and supplemental telephone or video assessment by off-site emergency physicians and full-service family physicians (FPs).
Concerns exist that telephone services can result in callers with minor issues being unnecessarily guided to attend an ED, and evidence exists that the addition of physician assessment can mitigate this.2,6 One goal of the HEiDi program was that, through an interprofessional approach involving both nurses and physicians, more 8-1-1 callers could be safely diverted from attending EDs than by involving nurses alone. In a previously published process evaluation, we found HEiDi virtual physicians subsequently advised 72.1% of nurse-triaged, urgently dispositioned callers away from visiting EDs or urgent care clinics within 24 hours, while advising 15.0% of callers to accelerate their nurse-assigned disposition and attend an ED immediately.7 Although outcomes after nurse consultation have been described in 1 setting, the effect of adding virtual physicians to a Canadian 8-1-1 line is unknown.5 Evaluating the effect of program changes on patient-oriented outcomes and health care use is essential for informed decision-making. However, this requires timely data access that is often difficult or impossible to secure.
This paper describes our use of a new BC Ministry of Health initiative, the Health Data Platform BC (HDPBC) to comprehensively analyze downstream health care use and the safety of the HEiDi service.8 We sought to explore the 24-hour and 7-day health care use and outcomes of 8-1-1 callers who were triaged by a nurse to seek immediate care and who were subsequently referred to HEiDi virtual physicians.
Methods
Study design
We conducted a descriptive analysis of routinely collected administrative health data between Nov. 16, 2020, and Apr. 30, 2021, following the Reporting of Studies Conducted Using Observational Routinely Collected Data (RECORD) statement.
Setting and study population
This study took place in BC, a Canadian province with more than 5 million residents across 5 regional health authorities.9 Callers of the 8-1-1 service who were referred by HealthLink BC navigators to nurses were evaluated with Healthwise, a widely used, algorithm-based software system that results in 7 triage dispositions.10 We use the term “caller” to refer to the individual for whom 8-1-1 was contacted; this is usually the person on the phone, but in a proportion of cases (and almost all pediatric cases), nurses and virtual physicians conversed initially or solely with a family member or caregiver.
The HEiDi program operated daily from 10 am to 10 pm (from study initiation through Jan. 3, 2021) or 9 am to 11 pm (from Jan. 4, 2021, to the study end). To be eligible for immediate subsequent assessment by a virtual physician during HEiDi operational hours, callers were required to be residents of BC with a provincial Personal Health Number (PHN), sufficient English-language proficiency (either the caller or a family member) as judged by the nurse and assigned a “RED-MD” disposition to seek immediate care (coded as “seek care now — MD/healthcare provider”). Immediate referral to a virtual physician was optional and at the discretion of nurses and consent of callers. After transfer to HEiDi, callers’ median wait-time was less than 30 minutes, as previously reported.7 In periods outside of HEiDi virtual physician hours, or when referrals were paused because of backlog, nurses managed callers independently.
Virtual physicians evaluated callers by phone or videoconferencing when deemed beneficial, providing them with advice and assigning 1 of 5 mutually exclusive dispositions with generally understood semantic meanings, as follows: “go to ED now” (i.e., proceed to the nearest appropriate ED without delay), “see primary care MD now” (i.e., typically within 24 h and ideally that day), “schedule an MD/HCP appointment” (i.e., within 1 wk), “try home treatment” (i.e., manage or observe condition at home) or “other” (i.e., any advice not captured by the previous categories, often involving “if/then” instructions). All RED-MD triaged callers who had a HEiDi encounter during the study period and a PHN were eligible. Further inclusion criteria and call-flow for 8-1-1 and HEiDi are provided in Appendix 1, Supplementary Material, available at www.cmajopen.ca/content/11/3/E459/suppl/DC1.
Research environment and data sources
In collaboration with the BC Ministry of Health, we used the newly launched HDPBC to identify ED visits, FP visits, hospital admissions and deaths.8 HealthLink BC provided a data extract of callers to the HDPBC in which records were anonymized with an encryption algorithm. Using the HDPBC’s secure research environment, we linked HEiDi caller records through their anonymized PHN to the National Ambulatory Care Reporting System (NACRS) for ED visits,11 the Discharge Abstract Database for hospital admission data,12 the Medical Services Plan for billings from fee-for-service physicians,13 the Vital Events Death for data on deaths14 and the Client Roster for demographic data.15 These data sources, and the approach we used to access and link them, are considered highly reliable and accurate.16
Variables and definitions
We obtained demographic characteristics, including caller sex, age, FP attachment, home health authority, economic dependency quintile, and rurality. We approximated caller age using year and month of birth, and categorized attachment to an FP by the number of FP encounters and the providers involved (Appendix 2, BC Ministry of Health algorithm, available at www.cmajopen.ca/content/11/3/E459/suppl/DC1). We categorized economic dependency quintiles from callers’ address-based dissemination area, a geographic proxy for deprivation,17 and rurality using callers’ Community Health Service Area.18
Nurses identified callers’ health concerns from a list of 23 topics, and we extracted caller disposition as assigned by the virtual physician from the HealthLink BC record. We obtained date and time of any subsequent ED visits from NACRS. Because not all BC EDs participate in NACRS, we also undertook a comprehensive search of the Discharge Abstract Database and Medical Services Plan to identify ED visits, following an approach described by the University of BC Centre for Health Services and Policy Research.19 We obtained the date and time of callers’ subsequent admissions to hospital from the Discharge Abstract Database, and subsequent visits to FPs from the Medical Services Plan by including claims with a specialty of family medicine and a service code corresponding to an in-office or telehealth FP visit, consultation or counselling. We obtained date of death for any callers with a record in the Vital Events Death database.
Linkage and analysis
For each 8-1-1 call record, we identified unique combinations of anonymized PHNs and call dates and times. For any anonymized PHN associated with multiple calls, we deemed the first call record within a 7-day period as the index call (thus, an individual would have multiple calls included only if they occurred more than 7 days apart). For each index call, we captured ED visits, hospital admissions, FP visits and deaths within 7 days as our primary outcomes of interest. We established the 7-day window a priori as a time frame within which subsequent service use or outcomes were likely linked to the issue prompting the index call. All 8-1-1 callers were successfully identified and linked in the HDPBC Client Roster demographic database.
We summarized variables and outcomes with descriptive statistics. For demographic and 8-1-1 call characteristics, we summarized callers in aggregate and noted counts of missing data. For service use and outcomes, we summarized callers overall and by virtual physician–assigned disposition for the 24-hour and 7-day periods after their index call. Given privacy requirements by the BC Ministry of Health regarding small cell sizes (n < 5), we were unable to report further on certain results.
We used SQL Server Management Studio (version 18.5, Microsoft) to query and link records across databases. We extracted eligible records and imported them to R (version 4.0, R Core Team) for statistical analysis.
Ethics approval
This study was approved by the University of British Columbia’s Clinical Research Ethics Board (H21-02209).
Results
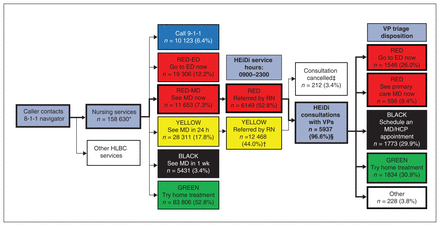
We identified 5937 RED-MD index calls to HEiDi during the study period, made by 5886 unique individuals. Of these, 927 (15.6%) calls used videoconferencing between the caller and HEiDi virtual physician, and the median virtual consultation length was 18.0 (interquartile range 13.0–24.0) minutes. Figure 1 depicts all calls to 8-1-1 during the study period and highlights the origin and disposition of our study population.
Overview of the flow of callers through 8-1-1 and the HealthLink BC Emergency iDoctors in Assistance (HEiDi) service during the study period (Nov. 16, 2020, through Apr. 30, 2021, inclusive). Thicker-weighted box outlines and arrows indicate the flow of callers specific to this study. Note: ED = emergency department, HCP = health care provider, HLBC = HealthLink BC, MD = medical doctor, RN = registered nurse, VP = virtual physician. *Number of nursing service calls are only for the HEiDi hours of 0900–2300 (previously 1000–2200 until Jan. 4, 2021). 8-1-1 nursing services also take calls outside of HEiDi’s hours. †Not included in study. ‡A consultation could be cancelled by the patient or HEiDi service for several reasons (e.g., caller or HEiDi disconnected, caller does not require service, incorrect record, no associated record). §This number indicates the number of caller encounters provided by HEiDi VPs and included in the study, excluding any referred callers who abandoned or cancelled their call before seeing the VP.
Demographic characteristics
Table 1 provides demographic characteristics of our study population, and illustrates that most HEiDi RED-MD callers were female and aged 20–64 years; 13.7% were calls for clients younger than 5 years, and 18.1% of callers were older than 64 years. About 15% of callers had a rural address and 60.4% were in the Fraser or Vancouver Coastal Health Authorities. Eighty-five percent of callers were attached to an FP, and 34.0% were in the lowest 2 economic dependency quintiles.
Participant characteristics
Health service use
Table 2 provides callers’ health service use, and illustrates that 60.8% of calls were triaged by HEiDi virtual physicians to a less urgent disposition than ascribed by nurses, including 1773 calls triaged to schedule an appointment with a health care provider and 1834 triaged to try a home treatment. Of those advised to try home treatment, 48.6% had no health system encounters over the next 7 days and 2.9% were admitted to hospital within 7 days. Of 1546 callers advised to go immediately to the ED, 62.8% had at least 1 ED visit within 24 hours and 9.2% had no further health system use within 7 days. Of 556 and 1773 callers advised to see a primary care provider right away or to schedule an appointment with a health care provider, 42.4% and 45.8%, respectively, had at least 1 FP visit within the next 7 days.
Callers’ health service use categorized by virtual physician disposition*
Mortality
At 1 week after calling, 8 callers of 5937 had died (0.1%), 5 of whom were among the 1546 callers advised to attend the ED immediately (0.3%). Six of the deaths occurred while callers were admitted to hospital. None of the 1834 callers who had been advised home management died.
Interpretation
We analyzed data from 5937 urgently triaged callers of a provincial nurse–managed, telephone service for health information, who were subsequently assessed by a virtual physician. Overall, at the completion of their HEiDi virtual consultation, most callers were triaged and advised to seek less urgent care options than an immediate ED or FP visit; more than 75% did not attend the ED over the next week. Importantly, among patients who were advised by a virtual physician to undertake home treatment, fewer than 3% were admitted to hospital within the following week and no patients died. Our results suggest that supplemental assessment by a virtual physician in a nurse-staffed 8-1-1 program can assist patients and families, and by extension, support the health care system by safely avoiding in-person assessment for a large proportion of urgently triaged callers.
Most telephone advice services employ nurses to manage consultations, and the demographics and presenting concerns of our study population are similar to those reported elsewhere.20 The impact of adding physicians to this type of service is poorly studied. A 2018 study in the United States found that, for callers with chest pain, physicians had shorter call durations than nurses (8 v. 16 min) and directed fewer callers to EDs (10% v. 16%).21 A 2015 study from England found that, of 1474 callers who would have been sent to an ED, FPs triaged only 27% to the ED.2 Numerous studies have found that most callers to nurse-managed systems follow the advice provided;22–24 however, this varies by both the suggested action and the caller’s condition. A 2010 Calgary study found callers were more likely to be concordant with advice to stay home than to go to an ED (83% v. 52%), and that callers with potential cardiac complaints were most likely to follow advice.5 Our results suggest similarities in caller concordance with virtual physician advice; however, multivariate analyses and explicit definitions are required for a fulsome understanding of factors associated with concordance, and the reasons for and impact of non-concordance.
Several of our findings were striking, and of potential interest for future research. For example, callers in the lowest economic quintiles were under-represented in our population. This suggests that access barriers may exist for the very group who are most likely to be frequent ED users.25 Furthermore, 85.0% of callers were categorized as “attached” to an FP, according to BC Ministry of Health’s algorithm. This is higher than previous self-reports,26 and could represent the unique nature of the population who accesses 8-1-1, or could be an artifact of how attachment is designated in the algorithm. More than 15% of callers in our study population were from a rural location, a figure slightly higher than the 11.8% of BC’s population living in rural communities.27 As a result of the positive ongoing results from HEiDi, Health-Link BC plans to sustain this service beyond the COVID-19 pandemic and continue to analyze its impact. In future work, we intend to investigate factors associated with concordance between advice given and subsequent service use,28 and to conduct an economic evaluation.
Timely data access is essential to support evidence-based quality improvement and is a strength of this study. Our multisectoral quality improvement team (including physicians, administrators, researchers, policy-makers, patient-partners and end-users) was able to rapidly access population data for this evaluation study, which allowed us to guide a major program and generate hypotheses for future investigation. However, in many jurisdictions, access to administrative data is complex, time-consuming and requires numerous permissions. Although intended to ensure privacy and security, challenges in data access have frequently not kept pace with innovations in computing and safe data sharing.29–31 Movements toward open data and democratization of information promise acceleration of the knowledge translation cycle.29,32 We hope the success of our proof-of-concept access to the HDPBC will form a foundation for future, near real-time analyses of outcome data to influence policy-making and clinical practice in BC, a vital component of a Learning Health System.33,34
Limitations
This study was undertaken in a public health care system with no cost to callers, potentially limiting generalizability. The lack of NACRS data from all BC EDs meant that, if relied on alone, some visits may have been missed, particularly in rural areas where EDs are less likely to contribute to NACRS data. However, we used best practices, developed in BC, to mitigate this through other approaches to identify ED visits.19 We conducted this study during the COVID-19 pandemic; thus, availability of FPs, urgent care clinics and EDs likely differed from historic norms and could have resulted in an increase in advice to attend an ED. In addition, because there was an increase in calls to 8-1-1 during the pandemic, there was likely a proportion of callers who terminated their calls because of longer wait times. Moreover, although the HEiDi program ran daily, it did not run 24 hours; thus, our findings may not be generalizable to overnight callers. In addition, the factors associated with the nurses’ decisions to refer 52.8% of RED-MD callers to virtual physicians are poorly understood. Virtual physicians had a range of training and experience, and were from various locations, potentially resulting in disposition variability. Moreover, the wording of the current virtual physician dispositions is not optimal to capture nuance or the generally understood application and meaning of those dispositions. This said, the key dispositions of “go to ED now” and “try home treatment” are unequivocal. Finally, we did not investigate callers’ disease characteristics and severity, and thus the association of these variables and downstream service use is unknown.
Conclusion
This descriptive study explored health service use and outcomes arising from the addition of virtual physicians to a provincial health information telephone service in Canada. Our findings suggest that supplementation with virtual physicians safely reduces the overall proportion of callers advised to seek urgent in-person care. Our results may be of interest to other jurisdictions who use a telephone triage service to avoid unnecessary in-person assessments.
Footnotes
Competing interests: Kendall Ho, Riyad Abu-Laban, Frank Scheuermeyer, Rina Chadha, Jim Christenson and John Tallon received professional fees from HealthLink BC for part-time work as virtual physicians with the HealthLink BC Emergency iDoctor in Assistance Program (HEiDi) during the course of this study. Kendall Ho and Rina Chadha receive additional funding from HealthLink BC for administration of the HEiDi program. No other competing interests were declared.
This article has been peer reviewed.
Contributors: All of the authors contributed to the conception and design of the work, and the acquisition, analysis and interpretation of data. All of the authors drafted the manuscript, revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: The HEiDi service and the evaluation of this virtual care pathway are funded by the British Columbia Ministry of Health through HealthLink BC (HLBC). The executive director of HLBC is a member of the steering committee and is a co-author for this publication.
Data sharing: Data reported here are available from the corresponding author on reasonable request to replicate our analysis. Requisite permissions must be obtained from HealthLink BC. Please contact the corresponding author to facilitate this process.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/3/E459/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- © 2023 CMA Impact Inc. or its licensors