Abstract
Summary
A United States-specific cost-effectiveness analysis, which incorporated the cost and health consequences of clinical fractures of the hip, spine, forearm, shoulder, rib, pelvis and lower leg, was undertaken to identify the 10-year hip fracture probability required for osteoporosis treatment to be cost-effective for cohorts defined by age, sex, and race/ethnicity. A 3% 10-year risk of hip fracture was generally required for osteoporosis treatment to cost less than $60,000 per QALY gained.
Introduction
Rapid growth of the elderly United States population will result in so many at risk of osteoporosis that economically efficient approaches to osteoporosis care warrant consideration.
Methods
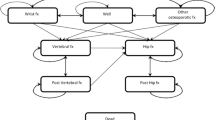
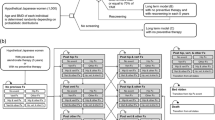
A Markov-cohort model of annual United States age-specific incidence of clinical hip, spine, forearm, shoulder, rib, pelvis and lower leg fractures, costs (2005 US dollars), and quality-adjusted life years (QALYs) was used to assess the cost-effectiveness of osteoporosis treatment ($600/yr drug cost for 5 years with 35% fracture reduction) by gender and race/ethnicity groups. To determine the 10-year hip fracture probability at which treatment became cost-effective, average annual age-specific probabilities for all fractures were multiplied by a relative risk (RR) that was systematically varied from 0 to 10 until a cost of $60,000 per QALY gained was observed for treatment relative to no intervention.
Results
Osteoporosis treatment was cost-effective when the 10-year hip fracture probability reached approximately 3%. Although the RR at which treatment became cost-effective varied markedly between genders and by race/ethnicity, the absolute 10-year hip fracture probability at which intervention became cost-effective was similar across race/ethnicity groups, but tended to be slightly higher for men than for women.
Conclusions
Application of the WHO risk prediction algorithm to identify individuals with a 3% 10-year hip fracture probability may facilitate efficient osteoporosis treatment.





Similar content being viewed by others
References
Kanis JA, Borgström F, De Laet C, Johansson H, Johnell O, Jönsson B, Odén A, Zethraeus N, Pfleger B, Khaltaev N (2005) Assessment of fracture risk. Osteoporos Int 16:581–589
Kanis JA, Black D, Cooper C, Dargent P, Dawson-Hughes B, De Laet C, Delmas P, Eisman J, Johnell O, Jönsson B, Melton L, Odén A, Papapoulos S, Pols H, Rizzoli R, Silman A, Tenenhouse A, International Osteoporosis F, National Osteoporosis F (2002) A new approach to the development of assessment guidelines for osteoporosis. Osteoporos Int 13:527–536
Anonymous (1998) Osteoporosis: review of the evidence for prevention, diagnosis and treatment and cost-effectiveness analysis. Introduction. Osteoporos Int 8(Suppl 4):S7–80
Department of Health and Human Services. (2004) In Bone Health and Osteoporosis A Report of the Surgeon General. Rockville, MD.
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005–2025. J Bone Miner Res 22:465–475
Sonnenberg FA, Beck JR (1993) Markov models in medical decision making: a practical guide. Med Decis Mak 13:322–338
Kanis JA, Odén A, Johnell O, Jönsson B, de Laet C, Dawson A (2001) The burden of osteoporotic fractures: a method for setting intervention thresholds. Osteoporos Int 12:417–427
Kanis JA, Borgström F, Zethraeus N, Johnell O, Odén A, Jönsson B (2005) Intervention thresholds for osteoporosis in the UK. Bone 36:22–32
Kanis JA, Johnell O, Odén A, Borgström F, Johansson H, De Laet C, Jönsson B (2005) Intervention thresholds for osteoporosis in men and women: a study based on data from Sweden. Osteoporos Int 16:6–14
Haentjens P, Autier P, Collins J, Velkeniers B, Vanderschueren D, Boonen S (2003) Colles fracture, spine fracture, and subsequent risk of hip fracture in men and women. A meta-analysis. J Bone Jt Surg Am Vol 85-A:1936–1943
Kanis JA, Johnell O, De Laet C, Johansson H, Odén A, Delmas P, Eisman J, Fujiwara S, Garnero P, Kroger H, McCloskey EV, Mellstrom D, Melton LJ, Pols H, Reeve J, Silman A, Tenenhouse A (2004) A meta-analysis of previous fracture and subsequent fracture risk. Bone 35:375–382
Melton LJ III, Crowson CS, O’Fallon WM (1999) Fracture incidence in Olmsted County, Minnesota: comparison of urban with rural rates and changes in urban rates over time. Osteoporos Int 9:29–37
United States Census Bureau (2005) State & County QuickFacts. (Accessed at http:quickfacts.census.gov/qfd/states/27/27109.html)
Cummings SR, Melton LJ (2002) Epidemiology and outcomes of osteoporotic fractures. Lancet 359:1761–1767
Cranney A, Wells G, Willan A, Griffith L, Zytaruk N, Robinson V, Black D, Adachi J, Shea B, Tugwell P, Guyatt G, Osteoporosis Methodology G, The Osteoporosis Research Advisory G (2002) Meta-analyses of therapies for postmenopausal osteoporosis. II. Meta-analysis of alendronate for the treatment of postmenopausal women. Endocr Rev 23:508–516
Borgström F, Johnell O, Kanis JA, Jönsson B, Rehnberg (2006) At what hip fracture risk is it cost-effective to treat? International Intervention thresholds for the treatment of osteoporosis. Osteoporos Int 17:1459–1471
Tosteson AN, Jönsson B, Grima DT, O’Brien BJ, Black DM, Adachi JD (2001) Challenges for model-based economic evaluations of postmenopausal osteoporosis interventions. Osteoporos Int 12:849–857
Badamgarav E, Fitzpatrick LA (2006) A new look at osteoporosis outcomes: the influence of treatment, compliance, persistence, and adherence.[comment]. Mayo Clin Proc 81:1009–1012
Tosteson AN (2003) Characterizing preferences for health outcomes in economic evaluations. J Rheumat Suppl 68:15–18
Hanmer J, Lawrence WF, Anderson JP, Kaplan RM, Fryback DG (2006) Report of nationally representative values for the noninstitutionalized US adult population for 7 health-related quality-of-life scores. Med Decis Mak 26:391–400
Gabriel SE, Tosteson AN, Leibson CL, Crowson CS, Pond GR, Hammond CS, Melton LJ 3rd (2002) Direct medical costs attributable to osteoporotic fractures. Osteoporos Int 13:323–330
Arias E, Anderson RN, Kung HC, Murphy SL, Kochanek KD (2003) Deaths: final data for 2001. Natl Vital Stat Rep 52:1–115
Melton LJ, III (2003) Adverse outcomes of osteoporotic fractures in the general population. J Bone Miner Res 18:1139–1141
Fisher ES, Baron JA, Malenka DJ, Barrett JA, Kniffin WD, Whaley FS, Bubolz TA (1991) Hip fracture incidence and mortality in New England. Epidemiology 2:116–122
Miller CW (1978) Survival and ambulation following hip fracture. J Bone Jt Surg Am Vol 60:930–934
Cooper C, Atkinson EJ, Jacobsen SJ, O’Fallon WM, Melton LJ 3rd (1993) Population-based study of survival after osteoporotic fractures. Am J Epidemiol 137:1001–1005
Katelaris AG, Cumming RG (1996) Health status before and mortality after hip fracture. Am J Public Health 86:557–560
Keene GS, Parker MJ, Pryor GA (1993) Mortality and morbidity after hip fractures.[see comment]. BMJ 307:1248–1250
Poor G, Atkinson EJ, O’Fallon WM, Melton LJ, III (1995) Determinants of reduced survival following hip fractures in men. Clin Orthop Relat Res 260–265
Magaziner J, Lydick E, Hawkes W, Fox KM, Zimmerman SI, Epstein RS, Hebel JR (1997) Excess mortality attributable to hip fracture in white women aged 70 years and older. Am J Public Health 87:1630–1636
Melton LJ III, Therneau TM, Larson DR (1998) Long-term trends in hip fracture prevalence: the influence of hip fracture incidence and survival. Osteoporos Int 8:68–74
Gold M, Siegel J, Russell L, Weinstein M (1996) Cost-effectiveness in Health and Medicine. Oxford University Press, New York
Center for the Evaluation of Value and Risk in Health (2007) CEA Registry. http://www.tufts-nemc.org/cearegistry/ Institute of Clinical Research and Health Policy Studies, Tufts New England Medical Center
Stone PW, Teutsch S, Chapman RH, Bell C, Goldie SJ, Neumann PJ (2000) Cost-utility analyses of clinical preventive services: published ratios, 1976–1997. Am J Prev Med 19:15–23
Dawson-Hughes B, Tosteson ANA, Melton LJ III, Baim S, Favus MJ, Khosla S, Lindsay RL (2008) Implications of absolute fracture risk assessment for osteoporosis practice guidelines in the U.S. Osteoporos Int DOI 10.1007/s00198-008-0559-5
Schousboe JT, Ensrud KE, Nyman JA, Melton LJ 3rd, Kane RL (2005) Universal bone densitometry screening combined with alendronate therapy for those diagnosed with osteoporosis is highly cost-effective for elderly women. J Am Geriatr Soc 53:1697–1704
Schousboe JT, Taylor BC, Fink HA, Kane RL, Cummings SR, Orwoll ES, Melton LJ 3rd, Bauer DC, Ensrud KE (2007) Cost-effectiveness of bone densitometry followed by treatment of osteoporosis in older men. JAMA 298:629–637
King AB, Saag KG, Burge RT, Pisu M, Goel N (2005) Fracture Reduction Affects Medicare Economics (FRAME): impact of increased osteoporosis diagnosis and treatment. Osteoporos Int 16:1545–1557
Kraemer DF, Nelson HD, Bauer DC, Helfand M (2006) Economic comparison of diagnostic approaches for evaluating osteoporosis in older women. Osteoporos Int 17:68–76
Guyatt G, Baumann M, Pauker S, Halperin J, Maurer J, Owens DK, Tosteson AN, Carlin B, Gutterman D, Prins M, Lewis SZ, Schunemann H (2006) Addressing resource allocation issues in recommendations from clinical practice guideline panels: suggestions from an American College of Chest Physicians task force. Chest 129:182–187
Kanis JA, Johnell O, Odén A, Borgström F, Zethraeus N, De Laet C, Jönsson B (2004) The risk and burden of vertebral fractures in Sweden. Osteoporos Int 15:20–26
Acknowledgements
The authors thank Dr. John Kanis for his insightful advice regarding this analysis. We also thank David Radley and Margaret Grove for their assistance with model development and analyses.
Conflicts of interest
None.
Funding
This study was supported by the National Osteoporosis Foundation. It was also supported in part by grants from the National Institutes of Health (AR048094 and AG12262).
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors comprise the National Osteoporosis Foundation Guide Committee.
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Tosteson, A.N.A., Melton, L.J., Dawson-Hughes, B. et al. Cost-effective osteoporosis treatment thresholds: the United States perspective. Osteoporos Int 19, 437–447 (2008). https://doi.org/10.1007/s00198-007-0550-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-007-0550-6